Mast Cell Activation (MCAS) Overview: Symptoms, Triggers, and Treatment
April 20, 2026

- MCAS is an immune condition caused by the sudden overactivation of mast cells. Triggers differ from person to person.
- Symptoms typically affect multiple body systems and range in severity.
- Treatment options include pharmaceutical antihistamines, medications for symptom management, and emergency epinephrine.
- Using symptom- and trigger-tracking tools like Human Health makes it easier to spot patterns, share data with your doctor, and make adjustments to your care plan.
For most people with allergies, reactions are caused by a clear trigger, like eating a peanut or getting stung by a bee. But that’s not the experience for people with mast cell activation syndrome (MCAS). Their story is much different, and it can be much more complicated.
Living with MCAS can feel like living with allergies, but the triggers are often broader and less predictable. The answers aren’t always straightforward. Management usually involves ongoing tracking and evolving treatment plans.
Caused by an overactivation of cells in the immune system, someone with MCAS can quickly go from feeling completely fine to having a strong allergic response in minutes. The reasons aren’t always clear.
In this article, we shed light on the key things you need to know about MCAS, from potential triggers and symptoms to the diagnostic process and your available treatment options.
Understanding MCAS
MCAS is an immunological condition that causes a person to experience repeated severe allergy symptoms. It is not considered an autoimmune condition, but it does impact how the immune system functions.
As part of the immune system, mast cells, which are a type of white blood cell, protect the body from pathogens, bacteria, viruses, and toxins. In people with MCAS, their mast cells activate in response to a trigger that they may or may not be aware of, releasing too many chemical mediators and causing multi-system allergic symptoms that range in intensity.
Because mast cells move around the body in the blood, symptoms are often widespread. They can impact the skin, the gastrointestinal system (stomach and intestines), the cardiovascular system (heart and blood vessels), the neurological system (brain, spine, and nerves), and the respiratory system (lungs and airway).
Severe MCAS reactions can occur, but they are not common.
Symptoms of MCAS
MCAS symptoms differ from person to person and are similar to the presentation of an allergic reaction.
Some common symptoms to look for include:
- Heart palpitations
- Chest pain
- A sudden drop in blood pressure
- Rash and itchy skin
- Skin flushing
- Hives
- Swelling of the face, lips, eyes, tongue, or throat
- Nasal congestion
- Abdominal pain
- Alternating constipation and diarrhea
- Nausea and vomiting
- Shortness of breath
- Brain fog and confusion
- Weakness
- Fainting
- Anaphylaxis
In rare severe cases, these symptoms can result in loss of consciousness, brain injuries, and possible death if left untreated. If you or someone you know has MCAS and is experiencing severe symptoms, immediately call emergency services or go to your local emergency room.
{{pro-tip-1}}
MCAS causes and triggers
One of the most frustrating parts of living with MCAS is that there are still lots of gaps in our clinical understanding of the condition.
MCAS is a recognized condition, but research is still evolving, and its diagnostic criteria continue to be refined. On top of this, the specific underlying mechanism of action that triggers the mast cells to become dysfunctional is not well understood.
Because symptoms can overlap with other conditions, MCAS can sometimes be misdiagnosed or overlooked.
All this means that individual tracking of symptoms and potential triggers is an essential part of MCAS management.
Triggers are classified into several categories: environmental, food, situational, and chemical. While every person experiences the condition differently, some commonly reported triggers of MCAS include:
- Sudden temperature changes
- Exposure to sunlight
- Emotional or physical stress
- Pain
- Physical exercise
- Fatigue
- Specific food or beverages, including alcohol
- Medications, including contrast dyes, antibiotics, and local anesthetics
- Perfumes and scents
- Environmental antigens, like dander, mold, and pollen
- Insect or reptile venoms, such as wasps, ants, spiders, snakes, and mosquitoes
- Infection and illnesses
How MCAS is diagnosed
An MCAS diagnosis requires multiple screening tests.
To be diagnosed, a physician will check whether you meet the following three criteria:
- Have ongoing symptoms of MCAS, affecting two or more organ systems
- Have laboratory results positive with an MCAS diagnosis
- Respond positively to treatment for mast cell activation
Your healthcare provider will start by asking you common screening questions, identifying your symptoms, and discussing your primary concerns.
{{pro-tip-2}}
Next, you’ll be sent for multiple rounds of blood work, looking for elevated levels of serum tryptase. Tryptase is the chemical enzyme released by mast cells when activated. If your blood work comes back with high tryptase, it can indicate that your mast cells are overactive.
Important note: Elevated tryptase does not always mean you have MCAS. Other underlying conditions may also cause this reading.
In addition to bloodwork, urine histamine testing, allergy tests, and a mast cell biopsy may also be ordered to finalize a diagnosis.
MCAS treatment options
If you or a loved one receives an MCAS diagnosis, you will have different pharmaceutical options available to you to help manage symptoms. If there is no improvement in your symptoms after receiving any of these treatments over time, your MCAS diagnosis should be reassessed.
Depending on your medical history and symptoms, medications your provider may prescribe include:
H1 antihistamines, including loratadine, cetirizine, and fexofenadine
H1 antihistamines are prescribed to manage itching, abdominal pain, skin flushing, headaches, and brain fog.
H2 antihistamines, including ranitidine and famotidine
H2 antihistamines help reduce gastrointestinal symptoms like nausea, constipation, diarrhea, and vomiting, while also supporting overall mast cell stability in people with MCAS.
Aspirin therapy
Aspirin therapy can be used to manage skin flushing, brain fog, and pain.
Do not start taking aspirin for your symptoms without consulting your physician first. Aspirin therapy requires close medical monitoring.
Mast cell stabilizers, like cromolyn sodium
Mast cell stabilizers like cromolyn sodium can reduce stomach and intestinal symptoms, including nausea, constipation, diarrhea, and vomiting.
Leukotriene inhibitors, including montelukast and zafirlukast
Leukotriene inhibitors are oral medications that help manage respiratory symptoms like wheezing and shortness of breath.
Emergency injectable epinephrine, including EpiPenⓇ
In the event of a severe MCAS reaction, emergency epinephrine can be injected to prevent the development of allergic anaphylaxis.
It is recommended that people with MCAS carry these emergency medications with them at all times.
Managing MCAS in real life
Besides using clinical treatment options, people living with MCAS can make lifestyle changes to improve their symptoms.
Eating a low-histamine diet
Some people with MCAS may have elevated histamine levels or be sensitive to histamine, so reducing dietary histamine can help reduce symptoms.
A low-histamine diet might look like this:
- Fresh, non-aged meat
- Salmon (fresh or flash frozen)
- Non-citrus fruits (apples, blueberries, mangoes, peaches, pomegranates)
- Gluten-free grains (amaranth, arrowroot, buckwheat, millet, rice, quinoa)
- Non-dairy milks (almond, coconut, hemp)
- Fresh vegetables
- Olive oil
- Coconut oil
- Almonds
- Potatoes
- Flax and chia seeds
- Butter and ghee
- Cream, cream cheese, and ricotta
- Soft cheeses that have not been aged or fermented
Not everyone with MCAS will notice a significant change in symptoms while eating this diet. To determine if it’s right for you, conduct a food experiment and diligently track your symptoms with the food you are eating to identify patterns.
Building a support system
The people in your life (family, friends, coworkers, and caregivers) should be aware of your condition. They should also be briefed on what to do if you have a sudden attack, including how to use injectable medications and how to call for emergency medical care.
Keeping a symptom journal
Since our understanding of MCAS and what causes it is still quite limited, keeping a daily journal is the best way to learn more about how your body reacts to triggers and treatments.
Everyone experiences MCAS differently, so tracking symptoms and potential triggers on a daily basis provides valuable information for your healthcare provider. They can use these insights to personalize your care plan.
{{inline-cta-1}}
Frequently asked questions:
What are mast cells?
Mast cells act as the body’s alarm system. As a type of white blood cell created in the bone marrow, they react to pathogens like bacteria and viruses to protect the body. In people with MCAS, they activate due to triggers that may or may not be known, causing symptoms.
What foods trigger MCAS?
There is no definitive list of foods that cause MCAS symptoms. Despite this, some people living with the condition find their symptoms ease when they eat a low-histamine diet.
What is the difference between histamine intolerance and MCAS?
Histamine intolerance is a proposed condition that impacts a person’s ability to digest the histamine they consume in food, causing allergy-like symptoms. However, it’s not currently acknowledged by the American Academy of Allergy and Immunology.
MCAS is a confirmed immune condition caused by the overactivation of mast cells in the body. It causes widespread allergy-like symptoms, often without a defined trigger.
Disclaimer: Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. The information in this guide is for educational purposes only and is not a substitute for professional medical care. Always consult your doctor or healthcare provider with questions about your health.
Sources:
- Mast Cell Activation Syndrome, Cleveland Clinic
- Histology, Mast Cells (2023)
- Mast cell activation syndrome, GARD Genetic and Rare Diseases Information Center
- Mast Cell Activation Disorders (2021)
- Mast cell activation syndrome: current understanding and research needs (2025)
- Symptoms and Triggers of Mast Cell Activation, The Mast Cell Disease Society
- Testing, The Mast Cell Disease Society
- Serum tryptase, Medscape
- Medications to Treat Mast Cell Diseases, The Mast Cell Disease Society
- Neuropsychiatric Manifestations of Mast Cell Activation Syndrome and Response to Mast-Cell-Directed Treatment: A Case Series (2023)
- Low histamine diet, John Hopkins Medicine
- Histamine intolerance: fact or fiction?, The American Academy of Allergy Asthma and Immunology
This is a div block with a Webflow interaction that will be triggered when the heading is in the view.

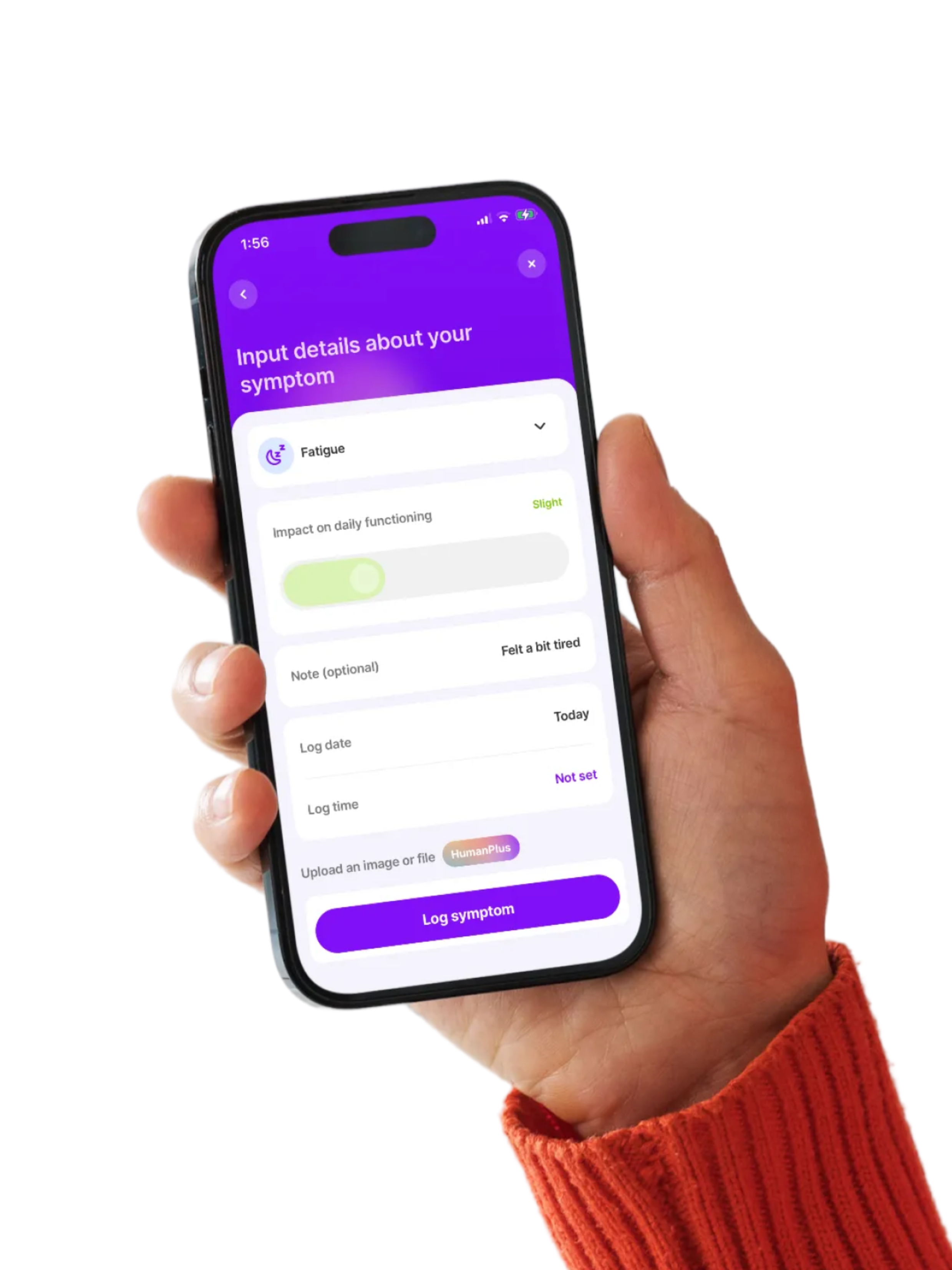
Want clearer answers over time?
For people with MCAS, tracking symptoms and triggers is key to managing the condition. The more you know, the easier it is to adjust your routine and treatment. Human Health lets you log symptoms, triggers, and responses to treatments, surface patterns, and create clear summaries to share with your provider.







Pro tip
If you’re unsure whether what you’re experiencing aligns with MCAS, start tracking your symptoms daily. Patterns are easier to see over a few weeks than in a single appointment.
Pro tip
Advocacy is a key part of MCAS management. Coming prepared to appointments with detailed observations and notes about your health is essential for getting the care you deserve.






.png)

