MCAS triggers: What to look for & how to manage them
March 18, 2026

- MCAS is an immune system condition that causes the sudden overactivation of mast cells, resulting in allergy-like symptoms without a clear cause.
- MCAS triggers differ from person to person. The best way to determine your potential triggers is by exposure testing and diligent tracking.
- While undergoing testing to determine your specific MCAS triggers, using a tracking app like Human Health makes it easier to spot patterns and share data with your doctor.
When someone has an allergy, treatment is mostly straightforward: as long as they avoid the allergen, they’ll avoid symptoms and a reaction.
It’s not that simple for people with mast cell activation syndrome (MCAS).
MCAS flare-ups can present for seemingly no reason at all, at any time. This reality is part of the reason identifying potential MCAS triggers is such a challenging process.
In this article, we want to help make this process less overwhelming: going deep on what MCAS is, sharing the most common MCAS triggers people experience, and suggesting how you can identify and track your own triggers to reduce the risk of a flare-up.
Let’s get into it.
What is mast cell activation syndrome?
MCAS is a rare condition that affects the immune system’s normal function. It is not considered to be an autoimmune disorder.
Mast cells, which are a type of white blood cell, are part of the body’s alarm system that flags when a foreign pathogen, like a virus or bacteria, has entered the body. When they come into contact with something they perceive as a threat, they release histamine. This triggers the inflammation cascade, causing allergy-like symptoms that affect nearby organs.
When working as expected, this system does not trigger without cause. But, in people with MCAS, their mast cells overactivate, releasing a higher amount of histamine throughout the body. As a result, they experience increased inflammation and are susceptible to strong allergy-like symptoms, often presenting without a clear trigger or cause.
Some of the most common symptoms of an MCAS flare-up are:
- A sudden drop in blood pressure
- Heart palpitations
- Chest pain
- Rashy and itchy skin
- Skin flushing
- Hives
- Swelling of the face, lips, eyes, tongue, or throat
- Nasal congestion
- Abdominal pain
- Alternating constipation and diarrhea
- Nausea and vomiting
- Shortness of breath
- Brain fog and confusion
- Weakness
- Fainting
In severe cases, people with MCAS can experience life-threatening symptoms of anaphylaxis.
If you or someone you know has MCAS and is experiencing severe symptoms that impact their ability to breathe or communicate, call 911 or go to the emergency room immediately.
Common MCAS triggers
Health experts still don’t fully understand the causes and triggers of MCAS, which can make managing the condition difficult and frustrating.
Currently, MCAS treatment primarily focuses on symptom management, helping people avoid potential triggers that lead to flare-ups. However, there are no universal MCAS triggers. Every person with the condition needs to take a trial-and-error approach to figuring out what works and doesn’t for reducing their symptoms.
For many, starting this process can be daunting. To make it easier, here’s a list of the most common MCAS triggers worth investigating:
{{pro-tip-1}}
Environmental MCAS triggers
Some people with MCAS notice an increase in their symptoms based on things in their surrounding environment. While these things cannot always be controlled, reducing exposure to environmental triggers can help lower symptom severity and frequency.
Examples of environmental triggers to consider include:
- Sudden changes in temperature, hot or cold
- Increased exposure to sunlight or UV radiation
- Insect or reptile venoms (wasps, ants, spiders, snakes, mosquitoes)
- Environmental antigens (dander, mold, pollen)
Food MCAS triggers
A large portion of potential MCAS triggers are diet-related.
Because people with MCAS have an elevated level of histamine in their bodies, monitoring your intake of dietary histamine could help reduce the severity of symptoms.
Histamine is a naturally occurring chemical in most foods, though some contain higher levels than others.
Foods known to be high in histamine or to cause a higher level of histamine release after consumption include:
- Aged and fermented cheese, like parmesan, blue cheese, and brie
- Alcoholic beverages
- Artificial colors and flavors
- Avocado and eggplant
- Kiwi, pineapple, papaya, strawberries, passionfruit, plums, and bananas
- Citrus fruits, like oranges, lemons, grapefruits, and limes
- Dried fruits
- Walnuts and cashews
- Certain seasonings, including all-spice, anise, cinnamon, chili powder, clove, curry powder, cayenne, MSG, nutmeg, and paprika
- Chocolate
- Eggs, especially raw
- Fermented foods like kimchi, sauerkraut, and yogurt
- Canned fish
- Flavored milk
- All leftovers that have not been frozen
- Legumes, including peanuts, soy beans, and chickpeas
- Licorice
- Pickles and vinegar-based condiments
- Probiotics
- Processed meats like jerky, pepperoni, and hot dogs
- Shellfish
- Sour cream and buttermilk
- Spinach, squash, and tomatoes
- Unpasteurized milk
- Wheat
Situational MCAS triggers
For some people with MCAS, symptoms worsen as a result of situational triggers in their day-to-day life. Many of these things can be unavoidable, but understanding your body’s connection to these triggers and your symptoms can help reduce flare-ups.
Examples of situations that can trigger an MCAS flare-up include:
- Emotional or physical stress
- Fatigue
- Physical exercise
- Infections or other illnesses
Chemical MCAS triggers
Occasionally, people with MCAS will notice worsened symptoms when exposed to specific chemical triggers. The severity of these flare-ups depends on the person, the extent and duration of exposure, and the chemical’s potency.
Some common examples of chemical triggers for MCAS include:
- Chemical odors (perfumes, gasoline, solvents, pesticides)
- Medications for treating MCAS or other medical conditions (NSAIDs, opiods, antibiotics, some local anesthetics)
- Contrast dyes for diagnostic procedures
How to manage your MCAS triggers
Because MCAS affects everyone differently, the burden of identifying triggers falls on the individual. Currently, most people with MCAS figure out their specific triggers by experimenting with exposures and recording their findings to identify patterns.
Keep a daily symptom and trigger journal
The best way to identify MCAS triggers is to have comprehensive data to track and analyze.
Most people find it difficult to identify what may be worsening their symptoms from memory alone.
Instead, it’s strongly recommended to keep a daily trigger and symptom journal. When you track how you feel day-to-day, including what you were exposed to (like high-histamine foods, pet dander, perfume), you can use that data to identify underlying patterns you and your healthcare team might otherwise miss.
Conduct a food experiment
If you’re curious about potential dietary triggers for your MCAS, conduct a food experiment. This is another great way to identify possible causes.
Follow these steps:
- Eat a low-histamine diet for 14 days.
- Track your symptoms during this time, recording what you eat and how you feel.
- After this period, slowly reintroduce high-histamine foods one-by-one, tracking symptoms.
Over time, this method will produce data you can use to identify foods that may be triggering your MCAS symptoms. You can then avoid them to make day-to-day life with MCAS easier.
{{inline-cta-1}}
Frequently asked questions
Is MCAS an autoimmune disorder?
MCAS is not an autoimmune disorder, but it is considered an immune disorder because it affects how a person’s immune system functions.
How do I figure out what my MCAS trigger foods are?
The best way to determine which foods trigger your MCAS symptoms is by conducting a 14-day food experiment.
Consume a low-histamine diet for 14 days. Record your symptoms and any potential triggers in the Human Health app. After this two-week period, slowly start adding high-histamine foods into your diet one at a time, recording your symptoms or reactions to determine which foods may be a trigger.
What kind of doctor treats MCAS?
If your primary care provider is considering an MCAS diagnosis, you will likely be referred to an allergy specialist or immunologist for further testing. Depending on your symptoms and their severity, you may also see a hematologist, dermatologist, gastroenterologist, and endocrinologist.
Disclaimer: Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. The information in this article is for educational purposes only and is not a substitute for professional medical advice. Please consult a qualified healthcare provider about your specific situation.
References:
- Mast Cell Activation Syndrome, Cleveland Clinic
- Mast cell activation syndrome: current understanding and research needs (2024)
- Symptoms and Triggers of Mast Cell Activation, The Mast Cell Disease Society
- Low histamine diet, John Hopkins Medicine
- Mast Cell Activation Syndrome (MCAS), American Academy of Allergy, Asthma & Immunology
- Mast cell activation syndrome: An up-to-date review of literature (2024)
- What initiates chemical intolerance? Findings from a large population-based survey of U.S. adults (2023)
This is a div block with a Webflow interaction that will be triggered when the heading is in the view.

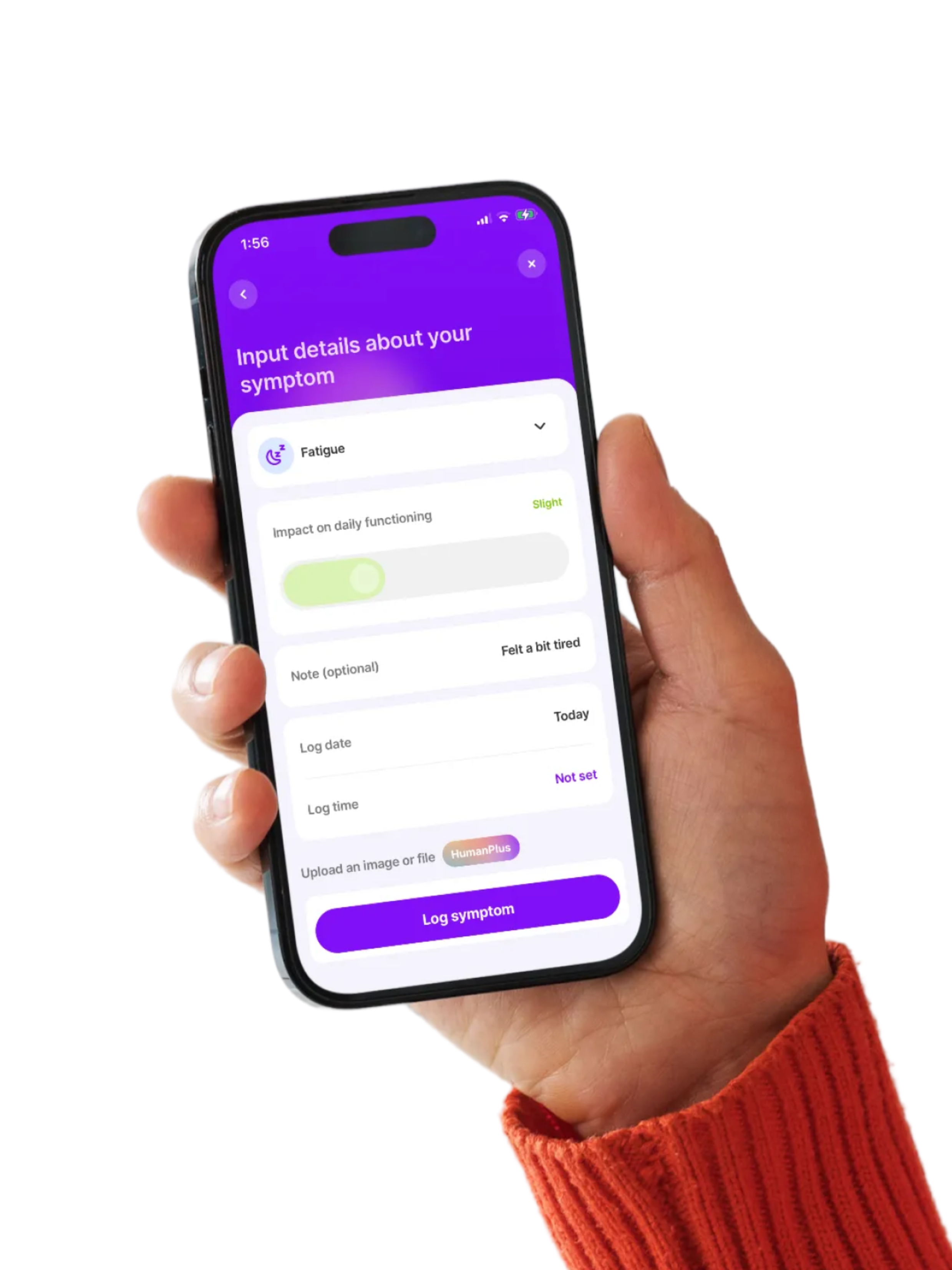
Stop guessing your triggers
Managing MCAS often comes down to identifying and avoiding your triggers. It can feel overwhelming at first, but tracking helps you spot patterns over time. With Human Health, you can log stress, diet, environment, and symptoms in one place, and turn that data into clear, doctor-ready summaries.







Pro tip
Triggers are often easier to identify when symptoms and exposures are logged together.






.png)

