Mast cell activation syndrome (MCAS) symptoms: What to look for and what to do
April 20, 2026

- MCAS is a condition caused by the overactivation of immune cells, resulting in unpredictable allergy-like symptoms. What triggers symptoms isn’t always obvious.
- Symptoms vary greatly in severity and type, but primarily affect the skin, gastrointestinal, cardiovascular, neurological, and respiratory systems. More than one body system is affected at the same time.
- Keeping a daily symptom journal using Human Health makes it easier to identify patterns, share information with your doctor, and better manage your condition.
For people living with mast cell activation syndrome (MCAS), managing symptoms and potential triggers can be as involved as a full-time job.
Because MCAS flare-ups can feel unpredictable at first, it can be difficult to anticipate when symptoms will appear or what might be driving them.
Many MCAS symptoms overlap with other conditions, so no single symptom on its own is usually enough to explain what’s happening. Instead, it’s the pattern of symptoms, often affecting multiple systems and occurring in episodes, that matters most.
Let’s get into it.
What is mast cell activation syndrome?
Mast cells, which are a type of white blood cell, act as the body’s alarm system to protect us from pathogens. MCAS is a condition that occurs when these immune system cells activate irregularly.
In people with MCAS, mast cells release large amounts of chemical mediators, triggering a widespread inflammatory response. This causes allergy-like symptoms and reactions that can be severe.
While MCAS does involve the immune system, it’s not considered an autoimmune disorder.
A frustrating part about living with MCAS is the current gaps in research. While the condition is recognized, our understanding of triggers and treatment options is still evolving. The condition can be diagnosed with established criteria, but these are still being refined and are not applied in all settings.
This developing knowledge means MCAS is sometimes overlooked or misdiagnosed. That’s why diligent tracking of your symptoms to identify patterns is an essential part of MCAS management.
MCAS symptoms: an overview
During an MCAS attack, the following steps occur to cause systemic allergic reactions:
- A trigger (known or unknown to the person) activates the mast cells.
- The mast cells release chemical mediators, including histamine.
- The mediators trigger the start of the inflammation cascade.
- This inflammation results in allergy-like symptoms throughout the body.
Important note: In rare cases, people with MCAS develop life-threatening symptoms of anaphylaxis. If you or someone you know with MCAS becomes disoriented, has difficulty breathing, or loses consciousness, call emergency services and get medical care immediately.
Skin symptoms of MCAS
Skin symptoms make up a large portion of MCAS reactions that are visibly detectable during a flare-up. Examples to look out for include:
- Itchiness
- Sweating
- Hyperthermia or hypothermia — a body temperature that’s too hot or too cold
- Flushing and redness
- Rashes
- Poor skin healing
- Bruising easily
Respiratory symptoms of MCAS
Many people with MCAS experience respiratory symptoms during an MCAS attack. Some of the most common airway and lung-based symptoms are:
- Dry cough
- Wheezing
- Swelling of the mouth and throat
- Chest tightness
- Difficulty breathing
Gastrointestinal symptoms of MCAS
The gastrointestinal symptoms associated with an MCAS attack can be uncomfortable. Examples to watch out for include:
- Abdominal pain
- Nausea
- Vomiting
- Diarrhea
- Constipation
- Bloating
- Difficulty swallowing
Neurological symptoms of MCAS
MCAS can cause inflammation of the neurological system, resulting in symptoms that last for the duration of the flare-up or longer. Some examples include:
- Headaches
- Migraines
- Fainting
- Seizures
- Brain fog and cognitive dysfunction
- Insomnia
- Restless legs
- Numbness and neuropathy (nerve pain)
Cardiovascular symptoms of MCAS
In extreme cases, an MCAS flare-up can impact the function of the heart. Cardiovascular symptoms include:
- Lightheadedness
- Sudden changes in blood pressure
- Heart palpitations
- Swelling and edema
- Chest pain
- Fast heart rate
Other associated MCAS symptoms
Some symptoms may be influenced by both mast cell activity and the broader effects of living with a chronic condition.
- Fatigue
- Change in appetite
- Weight loss or gain
- Anxiety
- Low mood
- Body pain
Having these symptoms doesn’t always mean you have MCAS
It’s important to note that just because you are experiencing some symptoms on the list above doesn’t necessarily mean you have MCAS.
However, because MCAS symptoms overlap with other health conditions, they can be easily misinterpreted. Tracking your symptoms and sharing that data with a physician is key to proper diagnosis.
How to get an MCAS diagnosis
According to current diagnostic criteria, to be diagnosed with MCAS, a person must:
- Have severe, recurring symptoms that impact at least two organ systems
- Have laboratory evidence that positively correlates with MCAS
- Respond to MCAS mediator targeting therapy
If you or someone you love has been experiencing an increase in allergy-like symptoms, booking an appointment with your care provider to ask about MCAS is the first step. Bringing a symptom journal to these appointments is a great way to advocate for your health needs and ensure no symptoms or concerns are forgotten.
Some of the most commonly asked questions during these appointments are:
- What symptoms have you been experiencing?
- How long have these symptoms been going on for?
- Are there things that make your symptoms worse? Does anything improve them?
- What treatment options have you explored to manage your symptoms?
If your doctor suspects that you may have MCAS, you will be sent for multiple rounds of blood work. Your serum tryptase will be assessed, as tryptase is the enzyme released by mast cells during activation.
Important note: Even if your bloodwork shows elevated serum tryptase, this does not necessarily mean you have MCAS. Other medical conditions can also cause the same result.
Other tests, including allergy testing, urine histamine tests, and bone marrow biopsies, may also be done to confirm a diagnosis of MCAS.
MCAS treatment and what to do next
If you or a loved one is diagnosed with MCAS, there are multiple treatment paths available to help manage symptoms.
Medications
Many people with MCAS take medications to stabilize their mast cell reactivity and manage symptoms during a flare-up.
Depending on your medical history and the symptoms you most commonly experience, you may be prescribed:
- H1 and H2 antihistamines
- Aspirin therapy
- Mast cell stabilizers
- Leukotriene inhibitors
For people with more severe symptoms, injectable epinephrine is prescribed as an emergency safety medication. This should only be used in emergencies if you or your loved one develop life-threatening symptoms of anaphylaxis.
Symptom and trigger journaling
A major part of MCAS management is tracking your health data to identify long-term patterns.
Because every person’s triggers are unique to them, many people living with MCAS can reduce the severity of their symptoms by taking specific medications or making changes to their lifestyle and diet.
Keeping a daily journal of symptoms alongside potential triggers can help to create a clearer picture of your condition and give you potential lifestyle changes to test.
Some of the most commonly reported potential MCAS triggers include:
- Sudden temperature changes
- Exposure to sunlight
- Emotional or physical stress
- Pain
- Physical exercise
- Fatigue
- Specific food or beverages, including alcohol
- Medications, including contrast dyes, antibiotics, and local anesthetics
- Perfumes and scents
- Venom from spider, wasp, snake, and mosquito bites
- Infection and illnesses
Human Health has over 1,000 trackable symptoms across more than 1,000 conditions you can log in the app, making it easier than ever to record and monitor changes in your health.
{{inline-cta-1}}
Frequently asked questions
What does an MCAS flare-up feel like?
MCAS symptoms vary from person to person. Depending on the severity of the symptoms, most people experience allergic-type reactions during an MCAS flare-up, including itchiness, flushing, abdominal pain, nausea, and more.
How do you know if you have MCAS?
Getting diagnosed with MCAS is a multi-step process.
First, your doctor will ask screening questions about your symptoms. Next, they will monitor your serum tryptase with blood work. They may also order urine histamine testing, allergy tests, or a bone marrow biopsy to confirm the diagnosis.
What is the difference between mastocytosis and MCAS?
Mastocytosis is a rare condition where the body produces too many mast cells. At this higher volume, abnormal variants of the cells build up and release extra histamine. As a result, people with mastocytosis have very strong allergic reactions to allergens.
MCAS is a condition caused by the overactivation of mast cells. It causes people to have allergy-like flare-ups, often without a clear trigger or cause.
Disclaimer: Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. The information in this guide is for educational purposes only and is not a substitute for professional medical care. Always consult your doctor or healthcare provider with questions about your health.
Sources:
- Mast Cell Activation Syndrome (MCAS), Cleveland Clinic
- Neuropsychiatric Manifestations of Mast Cell Activation Syndrome and Response to Mast-Cell-Directed Treatment: A Case Series (2023)
- What Mental Illness Is Associated With Mast Cell Activation Syndrome?, The EDS Clinic
- Using the Right Criteria for MCAS (2024)
- Serum Tryptase, Medscape
- Testing, The Mast Cell Disease Society
- Medications to Treat Mast Cell Diseases, The Mast Cell Disease Society
- Mastocytosis, Cleveland Clinic
This is a div block with a Webflow interaction that will be triggered when the heading is in the view.

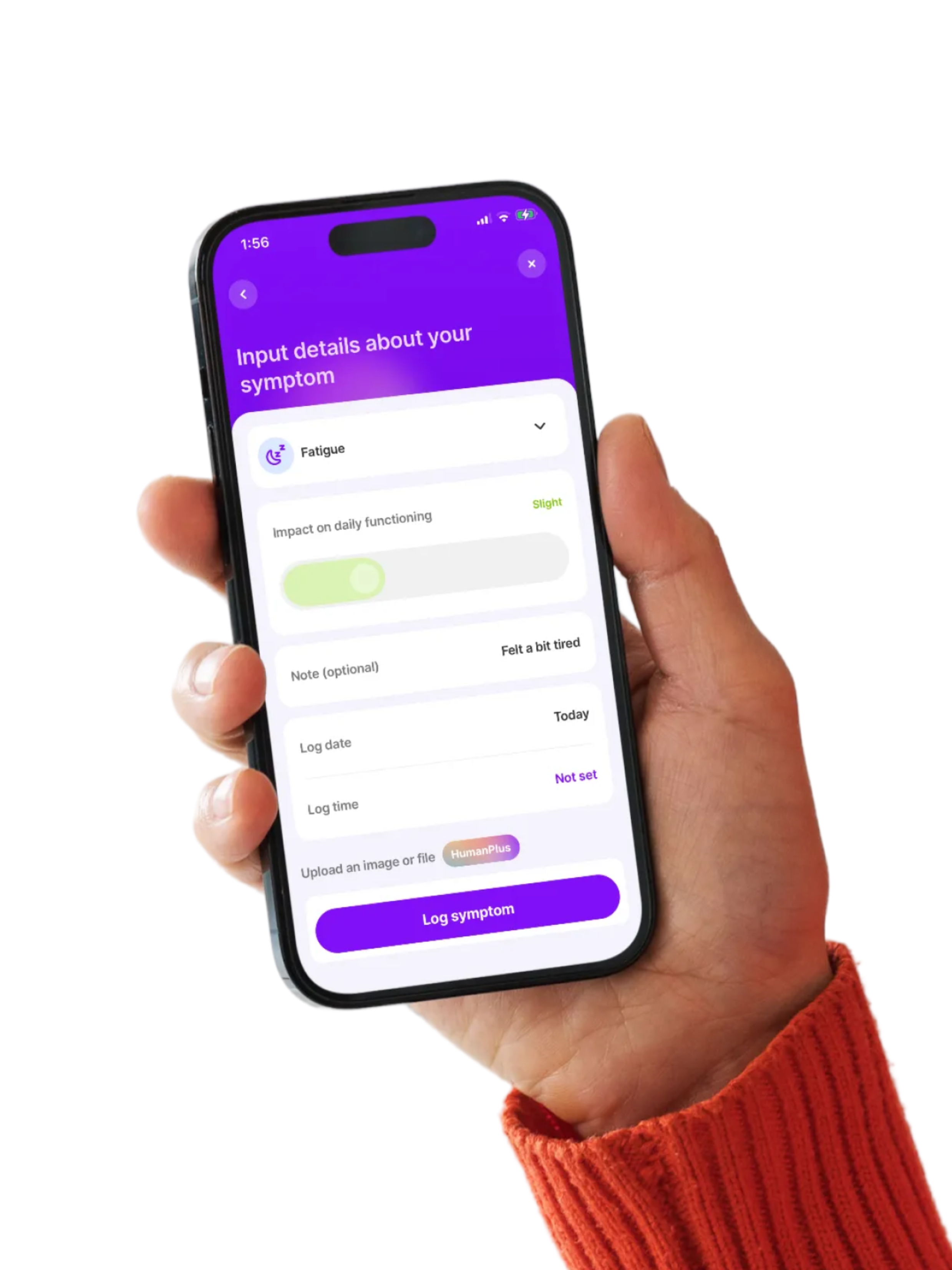
See how your symptoms connect
Living with MCAS means regularly tracking symptoms and triggers. The more you understand your patterns, the easier it is to personalize your care. Human Health helps you log daily changes, like energy, skin, gut symptoms, and flares, so you can spot trends and better manage your condition over time.







Pro tip
Symptoms can feel random day to day. Tracking them consistently can reveal patterns you might not notice in the moment.






.png)

