Systemic mastocytosis vs. mast cell activation syndrome (MCAS): What’s the difference?
April 24, 2026

- Despite having similar symptoms, diagnostic criteria, and treatments, systemic mastocytosis and MCAS are distinct medical conditions.
- In simple terms, systemic mastocytosis is caused by the body making too many mast cells, while MCAS is caused by the overactivation of mast cells.
- Symptom and trigger-tracking tools like Human Health make it easier to get an accurate diagnosis, monitor changes in your health, and share symptom patterns with your physician.
Systemic mastocytosis vs. mast cell activation syndrome (MCAS): What’s the difference between these conditions?
Despite having similar symptoms, diagnostic steps, and treatments, systemic mastocytosis and MCAS are separate medical conditions. Understanding that difference is essential for getting the quality of care you deserve.
Because both conditions can cause multi-system, allergy-like responses, tracking symptoms and potential triggers is a key part of ongoing management.
In this article, we shine a light on the main differences between systemic mastocytosis vs. MCAS, exploring everything you need to know about both so you are better informed when working with your doctor to get a diagnosis.
Here’s the breakdown.
What is systemic mastocytosis?
There are two broad types of mastocytosis.
Systemic mastocytosis, an acquired genetic disorder, is a rare immunological condition that causes the body to create too many mast cells. It differs from cutaneous mastocytosis, which primarily affects the skin in infants and toddlers.
Mast cells, which are a type of white blood cell, act as the body’s alarm system by releasing chemical mediators like histamine, tryptase, or leukotrienes when triggered. These mediators cause inflammatory responses.
In people with systemic mastocytosis, abnormal mast cells multiply. They collect throughout the body, building up in the organs and bone marrow. This can cause strong allergy-like symptoms and reactions, including anaphylaxis.
Types of systemic mastocytosis
There are different types of systemic mastocytosis, and they vary in severity.
Indolent systemic mastocytosis
The most common type of systemic mastocytosis. Indolent systemic mastocytosis primarily impacts the skin, but other organs may be involved. It can worsen progressively over time.
Smoldering systemic mastocytosis
Smoldering systemic mastocytosis can cause more severe multi-organ symptoms. These can directly impact the function of the body’s systems.
Bone marrow mastocytosis
This form of systemic mastocytosis affects only the bone marrow. It can cause severe allergic reactions, brittle bones, and osteoporosis.
In rare cases, people develop more advanced forms of systemic mastocytosis. Here 's a breakdown of these rare cases:
Systemic mastocytosis with myeloid/hematologic neoplasm
This type combines systemic mastocytosis with a blood or bone marrow condition, including cancer. This condition develops quickly and can cause significant organ damage.
Aggressive systemic mastocytosis
Can cause someone to develop more severe and long-lasting symptoms. It affects organ function and can cause damage over time.
Mast cell leukemia
This is the rarest and most aggressive form of systemic mastocytosis. It is considered a form of blood cancer.
What is mast cell activation syndrome (MCAS)?
Mast cell activation syndrome affects immune system function, but it’s not an autoimmune disorder.
With MCAS, you might experience recurring severe allergy symptoms due to the irregular activity of mast cells. In other words, while mastocytosis causes too many, or abnormal, mast cells in the body, MCAS causes the cells to overactivate.
As with mastocytosis, when triggered, the mast cells in people with MCAS release chemical mediators, which cause reactions in the body. At first, people rarely understand what specific trigger causes their immune system to react in this way. That’s why health tracking is so helpful.
The type, location, and severity of MCAS symptoms differ from person to person and can change over time. This makes managing the condition challenging.
Systemic mastocytosis vs. MCAS symptoms
Both systemic mastocytosis and MCAS can affect multiple systems in the body. These include the skin, gastrointestinal system (stomach and intestines), cardiovascular system (heart and blood vessels), respiratory system (lungs and airways), and nervous system (brain and nerves).
While the underlying cause of symptoms in systemic mastocytosis (too many mast cells) and MCAS (overactive mast cells) is different, many common symptoms overlap.
In systemic mastocytosis, symptoms can also vary depending on the subtype and whether specific organs are affected. In MCAS, symptoms tend to be more episodic and can change over time.
The most common symptoms of mastocytosis and MCAS include:
- A sudden drop in blood pressure
- Heart palpitations
- Chest pain
- Rashy and itchy skin
- Skin flushing
- Hives
- Swelling of the face, lips, eyes, tongue, or throat
- Nasal congestion
- Abdominal pain
- Alternating constipation and diarrhea
- Nausea and vomiting
- Shortness of breath
- Brain fog and confusion
- Weakness
- Syncope and fainting
In severe cases, a flare-up of mastocytosis or MCAS can cause a life-threatening anaphylactic reaction. If you or a loved one has either of these conditions and is having difficulty breathing or loses consciousness, call emergency services or go to your local emergency room immediately.
Diagnosing mastocytosis and MCAS
Multiple screening tests are needed to diagnose these conditions.
Your doctor will start by reviewing your health history and current symptoms. Keeping a detailed health journal of your symptoms is incredibly helpful for speeding up this process and ensuring no symptoms or triggers are forgotten.
From there, the diagnostic process depends on what your doctor suspects. Some tests look for an increased number of mast cells, while others look at how those cells are behaving
{{pro-tip-1}}
To diagnose systemic mastocytosis, doctors may look for:
- Clusters of abnormal mast cells in the bone marrow or other tissues
- Signs that these mast cells are behaving abnormally, such as specific markers or genetic changes
- Elevated levels of tryptase, a substance released by mast cells
Your doctor may order a series of different tests, including a skin biopsy, blood tests, ultrasounds to check if your spleen or liver is enlarged, and a DEXA body scan to check bone density.
A bone marrow biopsy is often required for systemic mastocytosis diagnosis.
The diagnostic criteria for MCAS are still being debated. But diagnosis generally involves the following three criteria:
- Ongoing symptoms of MCAS, affecting two or more organ systems
- Laboratory evidence that mast cells are being activated
- Positive response to treatment for mast cell activation
Your doctor may order blood work to test for elevated levels of serum tryptase. They may also send you for urine histamine testing, allergy tests, and a bone marrow biopsy.
Treatment options for mastocytosis and MCAS
Both systemic mastocytosis and MCAS are considered to be long-term conditions without a cure. Because of this, treatment is primarily focused on avoiding likely triggers, reducing symptom severity, and managing flare-ups.
Medications
The goal of medications for both conditions is to reduce the impact of histamine and other chemical mediators. Commonly prescribed medications include:
- H1 and H2 antihistamines
- Aspirin therapy
- Mast cell stabilizers
- Monoclonal antibodies
Other treatment options used to treat mastocytosis specifically include UV light therapy and stem cell (bone marrow) transplantation.
In some cases, particularly in more advanced forms of systemic mastocytosis, medications such as chemotherapy or targeted therapies may be used to reduce the number of mast cells.
Important note: Someone with MCAS or systemic mastocytosis can develop life-threatening anaphylaxis. It is strongly recommended that you carry injectable epinephrine with you at all times and train your loved ones and caregivers on how to use it in case of an emergency.
Eating a low histamine diet
Many people living with systemic mastocytosis or MCAS can ease their symptoms by eating a low-histamine diet.
Histamine naturally occurs in food. High-histamine foods include cured meats, fermented foods, aged cheeses, and citrus fruits. To help reduce your exposure to histamine and reduce the risk of flare-ups, eating low-histamine foods like fresh salmon, apples, and rice can be helpful.
Your doctor may recommend you complete a histamine food challenge, systematically cutting and re-introducing foods and tracking symptoms.
Important note: Not all people respond well to low-histamine diets. Some people can cut out high-histamine foods and still experience flare-ups. Others can eat them without issues. Trial and error and recording findings in a symptom and trigger journal are essential steps to better understand your specific reactions to food and other triggers.
Keeping a symptom journal
Because the symptoms of systemic mastocytosis and MCAS are sudden and can be severe, tracking them helps you better understand your body.
It is highly recommended that people with either condition track their symptoms to collect data about potential patterns. You can share this information with your doctor to better understand potential triggers and the effectiveness of treatment, and to evaluate your existing care plan.
{{inline-cta-1}}
Frequently asked questions
Is mastocytosis a form of leukemia?
The most common types of mastocytosis are not cancers. However, some advanced types of systemic mastocytosis can behave like cancerous conditions. For example, mast cell leukemia is a very rare form of blood cancer. If you notice any changes in your symptoms, speak to your doctor to conduct further assessments.
What does a mastocytosis flare feel like?
A mastocytosis flare-up feels similar to a sudden, intense allergic reaction. The symptoms a person feels often differ from attack to attack, but some of the most commonly reported symptoms include skin flushing, itchiness, hives, abdominal pain, swelling, shortness of breath, and gastrointestinal changes.
What causes mast cells to activate in MCAS?
The specific cause of the hyperactivation of mast cells in people with MCAS is not currently known. While there is no definitive cause, some commonly reported triggers for MCAS flare-ups include temperature changes, sunlight, pain, stress, physical exercise, fatigue, high-histamine foods, medications, and infections.
Disclaimer: Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. The information in this guide is for educational purposes only and is not a substitute for professional medical care. Always consult your doctor or healthcare provider with questions about your health.
Sources:
- Mastocytosis, Cleveland Clinic
- Cutaneous mastocytosis, Genetic and Rare Diseases Information Center
- Mastocytosis, Genetic and Rare Diseases Information Center
- Systemic mastocytosis, Mayo Clinic
- Mastocytosis, National Organization for Rare Disorders
- Mastocytosis (2013)
- Mast Cell Activation Syndrome, Cleveland Clinic
- Mast cell activation syndrome: current understanding and research needs (2025)
- Systemic mastocytosis (2023)
- Serum tryptase, Medscape
- Mast cell activation disorders (2021)
- Medications to Treat Mast Cell Diseases, The Mast Cell Disease Society
- Low histamine diet, John Hopkins Medicine
- Mast Cell Leukemia: An Update with a Practical Review (2023)
- Mastocytosis (2015)
This is a div block with a Webflow interaction that will be triggered when the heading is in the view.

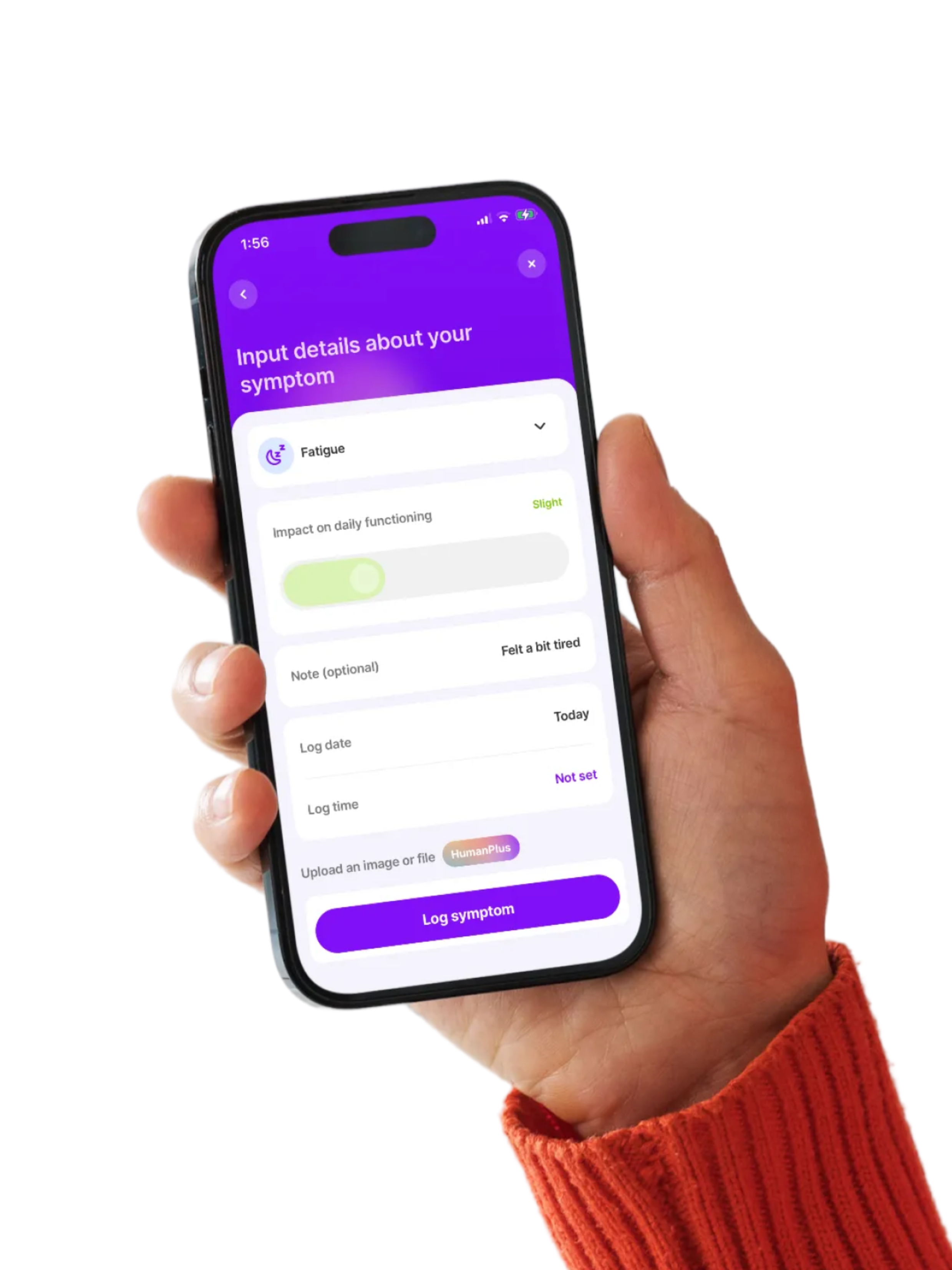
Get clarity while you wait
If you suspect systemic mastocytosis or MCAS, diagnosis isn’t always quick. These conditions are complex and affect people differently, so advocating for yourself matters. Tracking your symptoms and triggers can help. Human Health makes it easier to log frequency, severity, and timing to build a clearer picture.







Pro tip
If you’re navigating diagnosis, symptom tracking can help clarify patterns while you wait for specialist care.






.png)

