Magnesium for Fibromyalgia: Types, Benefits, Dosage & More
August 29, 2025

- Magnesium supports nerve and muscle function, energy production, and the nervous system, which may be especially relevant in fibromyalgia.
- Research is mixed: some studies suggest magnesium could support sleep, reduce fatigue, and ease pain, but larger, higher-quality trials are still needed.
- Different forms of magnesium (such as citrate, glycinate, malate, oxide, and threonate) vary in absorption and potential effects.
- Tracking magnesium intake and related symptoms with the Human Health app can reveal personal patterns to discuss with your healthcare provider.
Disclaimer: This article is for informational purposes only. Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before making changes to your supplements or care plan.
Living with fibromyalgia means carrying invisible weight: pain, fatigue, and restless nights that others rarely see.
While there’s no simple fix, some people explore magnesium as a way to support their body’s balance. This mineral fuels energy, soothes nerves, and steadies muscles — functions often disrupted in fibromyalgia.
In this guide, we’ll walk through the types of magnesium, what research says, and how you can safely track whether it makes a difference for you.
Magnesium’s role for people with fibromyalgia
Magnesium plays an important part in how your nerves and muscles work. Some early research (mostly from lab and animal studies) suggests it may help calm overactive nerve signals and may support the body’s natural relaxation system. This could help with muscle tension, pain sensitivity, and sleep, though more research in people with fibromyalgia is still needed.
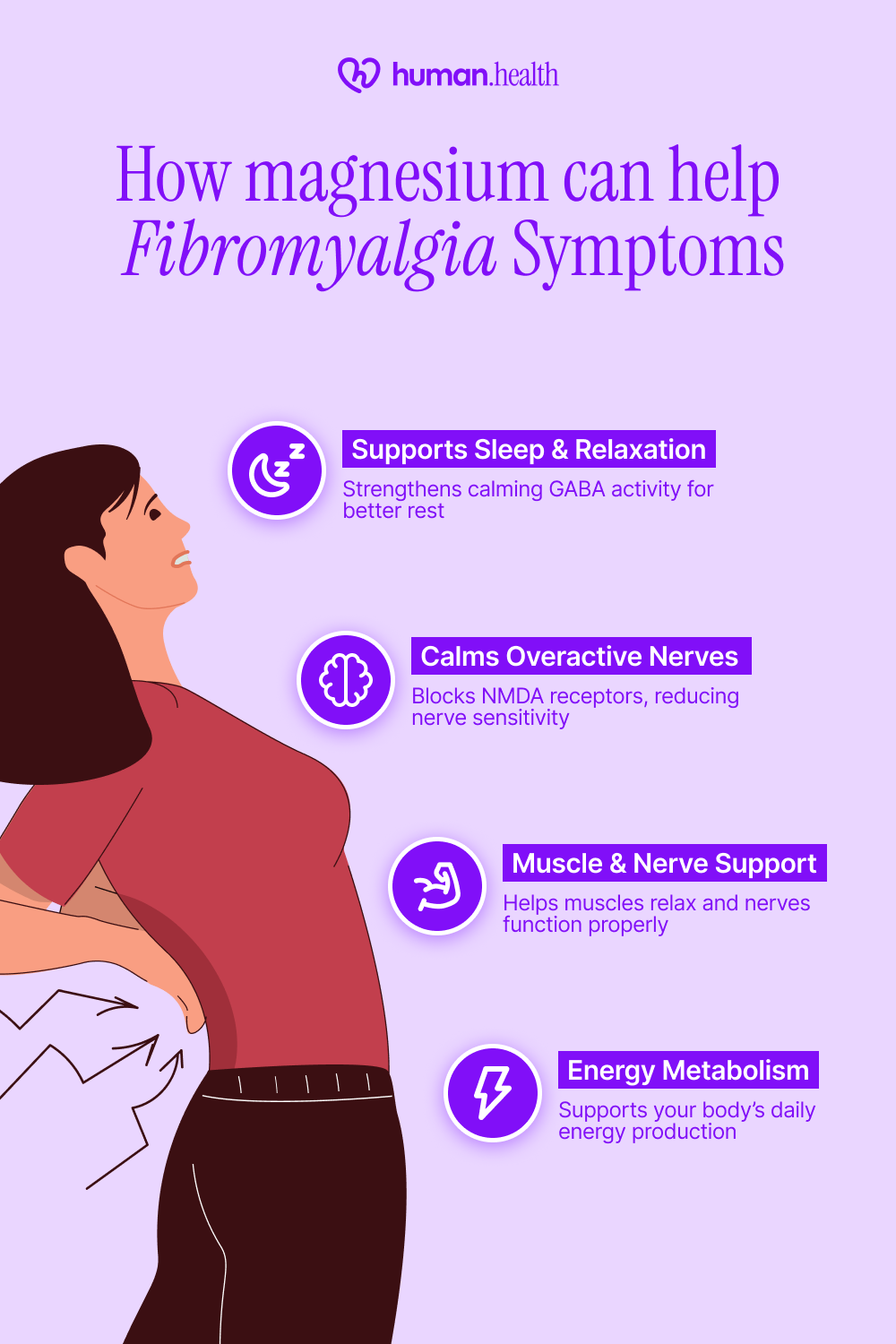
Types & forms of magnesium
Magnesium supplements come in several forms, and the way your body absorbs and responds to them can vary. Choosing the right type depends on your symptoms, digestive comfort, and personal tolerance. Here are some of the most commonly used forms.
Magnesium citrate
Magnesium citrate is one of the most common forms you’ll see on supplement shelves. Research has shown it tends to be absorbed well in the body, which is why it’s often used in studies and in practice. Because magnesium is important for both energy production and muscle function, some people with fibromyalgia choose citrate as a form that may be easier for the body to use.
Benefits
Magnesium citrate is absorbed well by the body and may support muscle and nerve health, which are important areas for people living with fibromyalgia. It can also have a mild laxative effect. This may be helpful for those dealing with constipation, though it may not suit everyone with sensitive digestion.
Magnesium glycinate
Magnesium glycinate combines magnesium with the amino acid glycine. This form is often gentler on the stomach because chelated versions like magnesium bisglycinate are absorbed more effectively than magnesium oxide.
Glycine also has calming effects that may support relaxation and better sleep, which is why some people choose this form to help with fibromyalgia-related restlessness. However, more research is needed to confirm these effects in people with fibromyalgia.
Benefits
Magnesium glycinate, also called bisglycinate, may be easier on the stomach and is sometimes used by people who struggle with sleep or anxiety. Small clinical studies suggest it could modestly improve sleep quality, especially in people with low magnesium intake, but more research is needed to confirm its role in fibromyalgia.
Magnesium oxide
Magnesium oxide is a widely available and inexpensive form, but it has lower absorption compared to other types.
Benefits
Magnesium oxide is absorbed less efficiently than many other forms, so it may not provide as much support for overall magnesium levels. It does have a stronger laxative effect, which some people find helpful for relieving constipation, though others may find it too harsh on digestion.
Magnesium threonate
Magnesium threonate is a newer form designed to cross the blood–brain barrier more effectively.
Benefits
Early studies suggest magnesium threonate may support cognitive health and memory. For people with fibromyalgia, it could be of interest for addressing “fibro fog” (issues with focus and mental clarity). Evidence is still emerging, and while initial findings are intriguing, larger and more rigorous studies are needed before its benefits are clear.
{{inline-cta-1}}
What the research says about magnesium’s effectiveness
Research on magnesium for fibromyalgia has produced mixed results. A 2021 literature review pulled together findings from multiple studies and found that while some showed lower magnesium levels in people with fibromyalgia (and correlations with more severe symptoms), others found no difference. Supplementation trials were also small and inconsistent, highlighting the need for larger, high-quality research.
2022 randomized controlled trial
A 2022 double-blind randomized trial tested magnesium chloride supplementation in 60 people with fibromyalgia. Participants who received magnesium reported better sleep quality and less fatigue, though pain relief was modest. Researchers cautioned that the short duration and small sample size limited how broadly the results could be applied.
2019 observational study
An observational study in 2019 with 53 women with fibromyalgia and 50 controls found that dietary magnesium intake was inversely related to pain intensity. However, blood magnesium levels did not differ between groups. As a cross-sectional study, it could not prove cause and effect, but it suggested a possible link worth exploring.
Signs you need magnesium
Low magnesium levels may contribute to a wide range of symptoms, many of which overlap with fibromyalgia. While only a doctor can confirm deficiency through testing, these common signs may suggest your body isn’t getting enough of this essential mineral.
#1. Muscle cramps and spasms
Because magnesium is essential for normal muscle contraction and relaxation, low levels can trigger cramps, involuntary contractions, or muscle spasms. Many people with fibromyalgia already deal with muscle tightness, and inadequate magnesium may make these sensations more frequent or harder to ease.
#2. Persistent fatigue
Magnesium plays a key role in how your body produces and uses energy. It helps enzymes that convert food into the energy your cells use for fuel. When magnesium levels are low, energy production may slow down, which can add to feelings of fatigue or weakness.
#3. Sleep difficulties
Magnesium supports relaxation by helping regulate calming brain signals, including GABA activity. This balance may improve sleep quality and make it easier to unwind before bed. Small clinical trials of magnesium L-threonate and magnesium bisglycinate have shown better sleep in adults with sleep problems, though larger studies are still needed.
#4. Headaches or migraines
Some studies link low magnesium to an increased risk of headaches and migraines. Magnesium helps blood vessels relax and regulates nerve signaling, both of which may influence head pain. For people with fibromyalgia who already experience frequent headaches, inadequate magnesium could make them more intense or harder to manage.
#5. Tingling or numbness
Magnesium supports normal nerve conduction. Low levels may disrupt how nerves send signals, sometimes producing numbness or tingling sensations in the hands, feet, or face. While fibromyalgia itself can cause unusual sensory experiences, magnesium deficiency may worsen or complicate these sensations.
{{inline-cta-2}}
#6. Mood changes
Magnesium interacts with neurotransmitters like serotonin and dopamine, which influence mood and emotional balance. Deficiency has been linked in several studies to increased anxiety, and some evidence also suggests associations with low mood. Because mood disturbances are already common in fibromyalgia, low magnesium may intensify feelings of restlessness, sadness, or stress.
#7. Irregular heartbeat
In more severe deficiencies, magnesium can affect the electrical activity of the heart, leading to arrhythmias (irregular heart rhythms). These disturbances are uncommon but potentially serious. Anyone with fibromyalgia who notices new or worsening irregular heartbeats should seek medical advice promptly rather than assume it’s part of their condition.
Symptom checklist:
Which ones apply to you?
- I get frequent muscle cramps or spasms
- I struggle with unexplained fatigue most days
- I have trouble falling or staying asleep
- I often experience headaches or migraines
- I sometimes feel tingling or numbness in my hands or feet
- I notice changes in my mood, like anxiety or irritability
- I’ve experienced palpitations or irregular heartbeat
Use the Human Health app’s daily symptom log to track patterns over time and share with your healthcare provider.
How to supplement safely and effectively
If you’re considering magnesium for fibromyalgia, it’s important to use it safely. Supplements may support muscle, nerve, and sleep health, but dosage, timing, and individual health factors matter. Always consult your healthcare provider before starting.
When to take magnesium
- Many people prefer taking magnesium at night to support relaxation and sleep.
- Others spread smaller doses throughout the day for better absorption.
- Timing often depends on your body’s tolerance and digestive comfort.
Safety considerations and who should avoid it
- Avoid magnesium supplements if you have chronic or severe kidney disease, as your body may not clear excess magnesium effectively, increasing the risk of toxicity.
- Check with your doctor if you take medications such as antibiotics, diuretics, or heart drugs, since interactions are possible (magnesium can reduce drug absorption or alter how these medicines work).
- Stop use and seek care if you experience diarrhea, nausea, low blood pressure, or irregular heartbeat.
Red flag warning box
Always talk to your healthcare provider before starting magnesium or any supplement. This is especially important if you:
- Have kidney disease or impaired renal function
- Are pregnant (should only be taken under medical supervision)
- Take multiple prescription medications
Track and remember with the Human Health app
Keeping up with supplements or medications can be tricky, especially if you’re juggling multiple prescriptions or therapies. The Human Health app includes a medication tracker and pill reminder, so you can log magnesium alongside other new treatments for fibromyalgia, stay consistent, and share a clear record with your healthcare provider.
Use the Human Health app to log symptoms, magnesium doses & flare patterns
Magnesium has been studied for fibromyalgia, with some evidence suggesting possible support for sleep, fatigue, and pain. But findings remain mixed, and effects vary from person to person.
The key is understanding how your own body responds over time.
With the Human Health app, you can log magnesium intake, track Fibromyalgia flare-ups, and record changes in sleep or energy. These daily notes create a clear, shareable record for your healthcare provider, helping you make more informed decisions based on both evidence and your personal experience.
Frequently Asked Questions:
#1. Can magnesium supplements interact with antidepressants or fibromyalgia medications?
Yes, magnesium can interact with certain antidepressants, muscle relaxants (like vecuronium), and other medications. Always check with your healthcare provider before adding supplements to your routine.
#2. Is it better to take magnesium in the morning or at night for fibromyalgia?
Many people prefer magnesium at night for relaxation and sleep support, but others split doses. The best timing depends on your body and doctor’s advice.
#3. Can I take magnesium during a fibromyalgia flare?
Yes, but its effects are not immediate. Tracking your intake and symptoms with the Human Health app can help you understand whether magnesium supports you during flare periods.
Sources:
- National Library of Medicine: The Role of Magnesium in Neurological Disorders
- National Library of Medicine: Magnesium and Fibromyalgia: A Literature Review
- National Library of Medicine: Effects of magnesium supplementation on muscle soreness in different type of physical activities: a systematic review
- National Library of Medicine: Magnesium-L-threonate improves sleep quality and daytime functioning in adults with self-reported sleep problems: A randomized controlled trial
- National Library of Medicine: Relation between magnesium and calcium and parameters of pain, quality of life and depression in women with fibromyalgia
- National Library of Medicine: Headaches and Magnesium: Mechanisms, Bioavailability, Therapeutic Efficacy and Potential Advantage of Magnesium Pidolate
- BMC Nutrition: Higher bioavailability of magnesium citrate as compared to magnesium oxide shown by evaluation of urinary excretion and serum levels after single-dose administration in a randomized cross-over study
- National Library of Medicine: Medical Treatment of Constipation
- National Library of Medicine: Bioavailability of magnesium diglycinate vs magnesium oxide in patients with ileal resection
- National Library of Medicine: Magnesium Bisglycinate Supplementation in Healthy Adults Reporting Poor Sleep: A Randomized, Placebo-Controlled Trial
- National Library of Medicine: Malic Enzyme Couples Mitochondria with Aerobic Glycolysis in Osteoblasts
- National Library of Medicine: Magnesium bioavailability from magnesium citrate and magnesium oxide
- Wisdom Library: Significance of Less bioavailability
- National Institutes of Health: Magnesium - Fact Sheet for Health Professionals
- National Library of Medicine: Magnesium Oxide in Constipation
- National Library of Medicine: The Effects of Magnesium Supplementation on Subjective Anxiety and Stress—A Systematic Review
- National Library of Medicine: Magnesium for the prevention and treatment of cardiovascular disease
- National Library of Medicine: Dietary Reference Intakes for Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride.
- National Library of Medicine: StatPearls - Magnesium Toxicity
- National Library of Medicine: Magnesium supplementation in pregnancy
- National Library of Medicine: Magnesium and Drugs
- National Library of Medicine: Magnesium sulfate enhances non-depolarizing muscle relaxant vecuronium action at adult muscle-type nicotinic acetylcholine receptor in vitro
Disclaimer: Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. The information on this site is intended to support, not replace, conversations with qualified healthcare professionals.
This is a div block with a Webflow interaction that will be triggered when the heading is in the view.

Keep Track of Your Condition
With the Human Health app - log and track everything; from symptoms to medications - everything in one place! Get updates and reminders & more.
Doctors Not Hearing You? Our App Does!
With the Human Health app, you can better understand what triggers you, your flares, and more. Gain real insights into how your treatment plan impacts your symptoms.







.jpg)





.png)

